An international team of clinicians and researchers have described the pathology of the novel coronavirus, or COVID-19, for the first time. Their findings were published by Tian et al in the Journal of Thoracic Oncology.
The article’s senior author, Shu-Yuan Xiao, MD, from the University of Chicago Medicine in Chicago, teamed up with a small group of clinicians from the Zhongnan Hospital of Wuhan University, in Wuhan, China.
Photo credit: Getty
The article describes two patients who recently underwent lung lobectomies for adenocarcinoma and were retrospectively found to have had COVID-19 at the time of surgery. Pathologic examinations revealed that, apart from the tumors, the lungs of both patients exhibited edema, proteinaceous exudate, focal reactive hyperplasia of pneumocytes with patchy inflammatory cellular infiltration, and multinucleated giant cells. Fibroblastic plugs were noted in airspaces.
“This is the first study to describe the pathology of disease caused by...COVID-19 pneumonia, since no autopsy or biopsies had been performed thus far. This would be the only description of early-phase pathology of the disease due to this rare coincidence...Since both patients did not exhibit symptoms of pneumonia at the time of surgery, these changes likely represent an early-phase of the lung pathology of COVID-19 pneumonia," Dr. Xiao said.
Two Cases
The first case was an 84-year-old female patient who was admitted for treatment evaluation of a tumor measuring 1.5 cm in the right middle lobe of the lung. The tumor was discovered on chest computed tomography scan at an outside hospital. She had a past medical history of hypertension for 30 years, as well as type 2 diabetes. Despite comprehensive treatment, assisted oxygenation, and other supportive care, the patient’s condition deteriorated, and she died. Subsequent clinical information confirmed that she was exposed to another patient in the same room who was subsequently found to be infected with the 2019 novel coronavirus.
The second case was a 73-year-old male patient who presented for elective surgery for lung cancer, which presented as a small mass in the right lower lobe of the lung. He had a past medical history of hypertension for 20 years, which had been adequately managed. Nine days after lung surgery, he developed a fever with dry cough, chest tightness, and muscle pain. A nucleic acid test for COVID-19 came back as positive. He gradually recovered and was discharged after 20 days of treatment in the infectious disease unit.
Common Scenario
According to the study, these two incidences also typify a common scenario during the earlier phase of the COVID-19 outbreak, during which a significant number of health-care providers became infected in hospitals in Wuhan, and patients in the same hospital room were cross-infected as they were exposed to unknown infectious sources. The presence of early lung lesions days before the patients developed symptoms corresponds to the long incubation period (usually 3 to 14 days) of COVID-19.
The long incubation period made it difficult to prevent transmission during the early days of this outbreak, as many health-care workers in Wuhan became infected when they were seeing patients without sufficient protection, according to Dr. Xiao. As of today, more than 15 doctors in Wuhan have died of COVID-19.
“We believe it is imperative to report the findings of routine histopathology for better understanding of the mechanism by which [COVID-19] causes lung injury in the unfortunate tens and thousands of patients in Wuhan and worldwide,” said Dr. Xiao.
Further studies by Dr. Xiao’s team and collaborators on COVID-19 pathology through postmortem biopsies are ongoing, which should provide data on the late changes of this disease.
Editor's note: Find the latest COVID-19 news and guidance in Medscape's Coronavirus Resource Center.
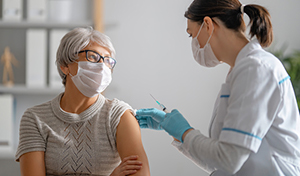
The CDC has issued updated guidance for people with underlying medical conditions who are considering getting the
coronavirus vaccine.
"Adults of any age with certain underlying medical conditions are at increased risk for severe illness from the virus that causes
COVID-19," the CDC said in the guidance posted on Saturday. "mRNA COVID-19 vaccines may be administered to people with
underlying medical conditions provided they have not had a severe allergic reaction to any of the ingredients in the vaccine."
Both the Pfizer and Moderna vaccines use mRNA, or messenger RNA.
The CDC guidance had specific information for people with HIV, weakened immune systems, and autoimmune conditions such
as Guillain-Barre syndrome and Bell's palsy who are thinking of getting the vaccine.
People with HIV and weakened immune systems "may receive a COVID-19 vaccine. However, they should be aware of the
limited safety data," the CDC said.
There's no information available yet about the safety of the vaccines for people with weakened immune systems, the CDC said.
People with HIV were included in clinical trials, but "safety data specific to this group are not yet available at this time," the CDC
said.
Cases of Bell's palsy, a temporary facial paralysis, were reported in people receiving the Pfizer and Moderna vaccines in clinical
trials, the FDA said Dec. 17.
But the new CDC guidance says the FDA "does not consider these to be above the rate expected in the general population.
They have not concluded these cases were caused by vaccination. Therefore, persons who have previously had Bell's palsy
may receive an mRNA COVID-19 vaccine."
Researchers have determined the vaccines are safe for people with GBS, a rare autoimmune disorder in which the body's
immune system attacks nerves just as they leave the spinal cord, the CDC said.
"To date, no cases of Guillain-Barre syndrome (GBS) have been reported following vaccination among participants in the mRNA
COVID-19 vaccine clinical trials," the CDC guidance says. "With few exceptions, the independent Advisory Committee on
Immunization Practices (ACIP) general best practice guidelines for immunization do not include a history of GBS as a
precaution to vaccination with other vaccines."
For months, the CDC and other health authorities have said that people with certain medical conditions are at an increased risk
of developing severe cases of COVID-19.
Sources:
CDC: "COVID-19 Vaccination Considerations for Persons with Underlying Medical Conditions"
Now that COVID-19 vaccines are being distributed, the American Association for Cancer Research (AACR) has called for
people with cancer to be considered as a high priority group.
"The available evidence supports the conclusion that patients with cancer, in particular with hematological malignancies, should
be considered among the high-risk groups for priority COVID-19 vaccination," says the AACR's COVID-19 and Cancer Task
Force.
A review of literature suggests that COVID-19 fatality rates for patients with cancer were double that of individuals without
cancer, the team notes. The higher mortality rates still trended upward, even after adjusting for confounders including age, sex,
and comorbidities, indicating that there is a greater risk for severe disease and COVID-19 related mortality.
The new AACR position paper was published online December 19 in Cancer Discovery.
"We conclude that patients with an active cancer should be considered for priority access to COVID-19 vaccination, along other
particularly vulnerable populations with risk factors for adverse outcomes with COVID-19," the team writes.
However, the authors note that "it is unclear whether this recommendation should be applicable to patients with a past diagnosis
of cancer, as cancer survivors can be considered having the same risk as other persons with matched age and other risk
factors.
"Given that there are nearly 17 million people living with a history of cancer in the United States alone, it is critical to understand
whether these individuals are at a higher risk to contract SARS-COV-2 and to experience severe outcomes from COVID-19,"
they add.
Allocation of Initial Doses
There has already been much discussion on the allocation of the initial doses of COVID-19 vaccines that have become available
in the US. The Advisory Committee on Immunization Practices (ACIP) of the Centers for Disease Control and Prevention (CDC)
recommended that the first wave of vaccinations, described as Phase 1a, should be administered to US healthcare workers
(about 21 million people) and residents of long-term care facilities (about 3 million).
The next priority group, Phase 1b, should consist of front-line essential workers, a group of about 30 million, and adults aged 75
years or older, a group of about 21 million. When overlap between the groups is taken into account, Phase 1b covers about 49
million people, according to the CDC.
Finally, Phase 1c, the third priority group, would include adults aged 65-74 years (a group of about 32 million), adults aged 16-64
years with high-risk medical conditions (a group of about 110 million), and essential workers who did not qualify for inclusion in
Phase 1b (a group of about 57 million). With the overlap, Phase 1c would cover about 129 million people.
"Cancer is one of the categories of individuals at high risk," said Antoni Ribas, MD, PhD, AACR president and chair of the AACR
COVID-19 and Cancer Task Force. "At the ACIP vote on December 20, the priority access was assigned to Phase 1c, but this
results in a potential significant delay in vaccination for the particularly vulnerable population of patients with cancer at this time
of highest risk, with the winter worsening of the COVID-19 pandemic."
"Any delay in vaccine access will result in loss of life that could be prevented with earlier access to vaccination," Ribas told
Medscape Medical News.
He noted that the task force agrees that people whose work is essential to run society should receive priority vaccination, but
consideration should be given to first vaccinating patients with cancer who are at increased risk of dying if they get COVID-19.
"This would include the 2 or 3 million people in the US who currently are receiving treatments for cancer, in particular if they
have blood cancers or lung cancer, as they are at a particularly higher risk of dying based on the studies we reviewed," he said.
Patients With Cancer a 'High Priority' for
COVID-19 Vaccine
1/4/2021 https://www.medscape.com/viewarticle/943308_print
https://www.medscape.com/viewarticle/943308_print 2/3
"Moreover, a subset of cancer patients appears to have prolonged viral shedding, placing their healthcare providers and
caregivers at higher risk."
The best scenario, Ribas emphasized, "would be that with two approved COVID-19 vaccines there is enough stock in the next
few weeks to vaccinate all individuals assigned to Phase 1b and 1c."
Questions Remain
Approached for independent comment, Cardinale Smith, MD, PhD, chief quality officer for cancer services for the Mount Sinai
Health System in New York City, agreed with the AACR task force. "I share that they should be high priority," she said, "But we
don't know that the efficacy will the same."
Smith noted that the impact of cancer therapy on patient immune systems is more related to the type of treatment they're
receiving, and B and T cell responses. "But regardless, they should be getting the vaccine, and we just need to follow the
guidelines," she said.
The AACR task force notes that information thus far is quite limited as to the effects of COVID-19 vaccination in patients with
cancer. In the Pfizer-BioNTech BNT162b2 COVID vaccine trial, of 43,540 participants, only 3.7% were reported to have cancer.
"It is clear that we need more data and specific studies in patients with cancer, but this should not delay access to priority
vaccination," said Ribas. "There is considerable experience with other vaccines, such as the yearly flu vaccine, in cancer
patients with very good safety records."
Other large COVID-19 vaccine trials will provide further follow-up information on the effectiveness of the vaccines in patients
receiving different cancer treatments, they write, but for now, there is "currently not enough data to evaluate the interactions
between active oncologic therapy with the ability to induce protective immunity" to COVID-19 with vaccination.
Ribas pointed out that studies of natural immune response to COVID-19 have documented that patients with hematologic
malignancies have a suboptimal ability to mount an immune response to the virus. This results in these patients having a
"remarkably" high risk of fatality compared with other patient populations with COVID-19 infection.
"The fact that the antibody and T-cell responses to the COVID-19 vaccines are higher than in many individuals with natural
COVID-19 infection provides an even stronger rationale to offer vaccination to persons with lower immune responses to the
virus," he said. "Although ongoing studies will provide more information about how to best protect cancer patients with vaccines,
at present, there is no evidence that the vaccine should be delayed in cancer patients.
"Of course, patients with cancer should consult with their healthcare providers about their potential risks and benefits to decide
whether getting vaccinated is right for them," he added.
In a recent interview with Medscape Medical News, Nora Disis, MD, a medical oncologist and director of both the Institute of
Translational Health Sciences and the Cancer Vaccine Institute, University of Washington, Seattle, also discussed vaccinating
cancer patients.
She pointed out that even though there are data suggesting that cancer patients are at higher risk, "they are a bit murky, in part
because cancer patients are a heterogeneous group."
"For example, there are data suggesting that lung and blood cancer patients fare worse," said Disis, who is also editor-in-chief of
JAMA Oncology. "There is also a suggestion that, like in the general population, COVID risk in cancer patients remains driven
by comorbidities."
She also pointed out the likelihood that individualized risk factors including the type of cancer therapy, site of disease, and
comorbidities "will shape individual choices about vaccination among cancer patients."
It is also reasonable to expect that patients with cancer will respond to the vaccines, even though historically some believed that
they would be unable to mount an immune response. "Data on other viral vaccines have shown otherwise," said Disis. "For
example, there has been a long history of studies of flu vaccination in cancer patients, and in general, those vaccines confer
protection."
Several of the authors of the AACR position paper, including Ribas, report relationships with industry as detailed in the paper.
Editor's note: Find the latest COVID-19 news and guidance in Medscape's Coronavirus Resource Center.
Anthony Fauci, MD, says the coronavirus pandemic may get worse in coming months, including a post-holiday surge in cases.
In an interview on CNN, Fauci was asked if he thought "the worst was yet to come." He said, "I do."
"We very well might see a post-seasonal ― in the sense of Christmas, New Year's ― surge, and, as I have described it, as a
surge upon a surge," said Fauci, the director of the National Institute of Allergy and Infectious Diseases.
Fauci said holiday travel could cause a spike in cases. Besides exposing themselves at airports, travelers usually mix
households when they arrive at their destinations, he said. Even though health authorities urge people not to travel, "it’s going to
happen," Fauci said.
"We are really at a very critical point. ... So I share the concern of President-elect (Joe) Biden that as we get into the next few
weeks, it might actually get worse," Fauci said.
Biden recently said that the "darkest days" in the coronavirus pandemic are ahead and urged Americans to prepare themselves
for a difficult struggle. Fauci has agreed to serve as Biden’s top health adviser.
December has already been the hardest month for the COVID-19 pandemic in the United States.
More than 65,000 people have died of coronavirus-related reasons so far this month, compared to only about 37,000 in
November, according to the Covid Tracking Project. Hospitalizations are up, with more than 100,000 people in the hospital per
day since Dec. 2.
Overall, there have been more than 19 million confirmed cases in the United States and more than 333,000 COVID-related
deaths ― the most of any nation in the world.
COVID-19 vaccinations should bring the pandemic under control, but it will take many months for the United States to develop
herd immunity, Fauci said. Health care workers and residents of long-term care facilities are the top priority groups receiving the
vaccine.
"I hope that by the time we get to the fall we will reach that critical percentage of people that we can really start thinking about a
return to some form of normality," Fauci said.
Fauci, who just turned 80, got a COVID-19 vaccination recently. He said he had no side effects besides arm soreness for about